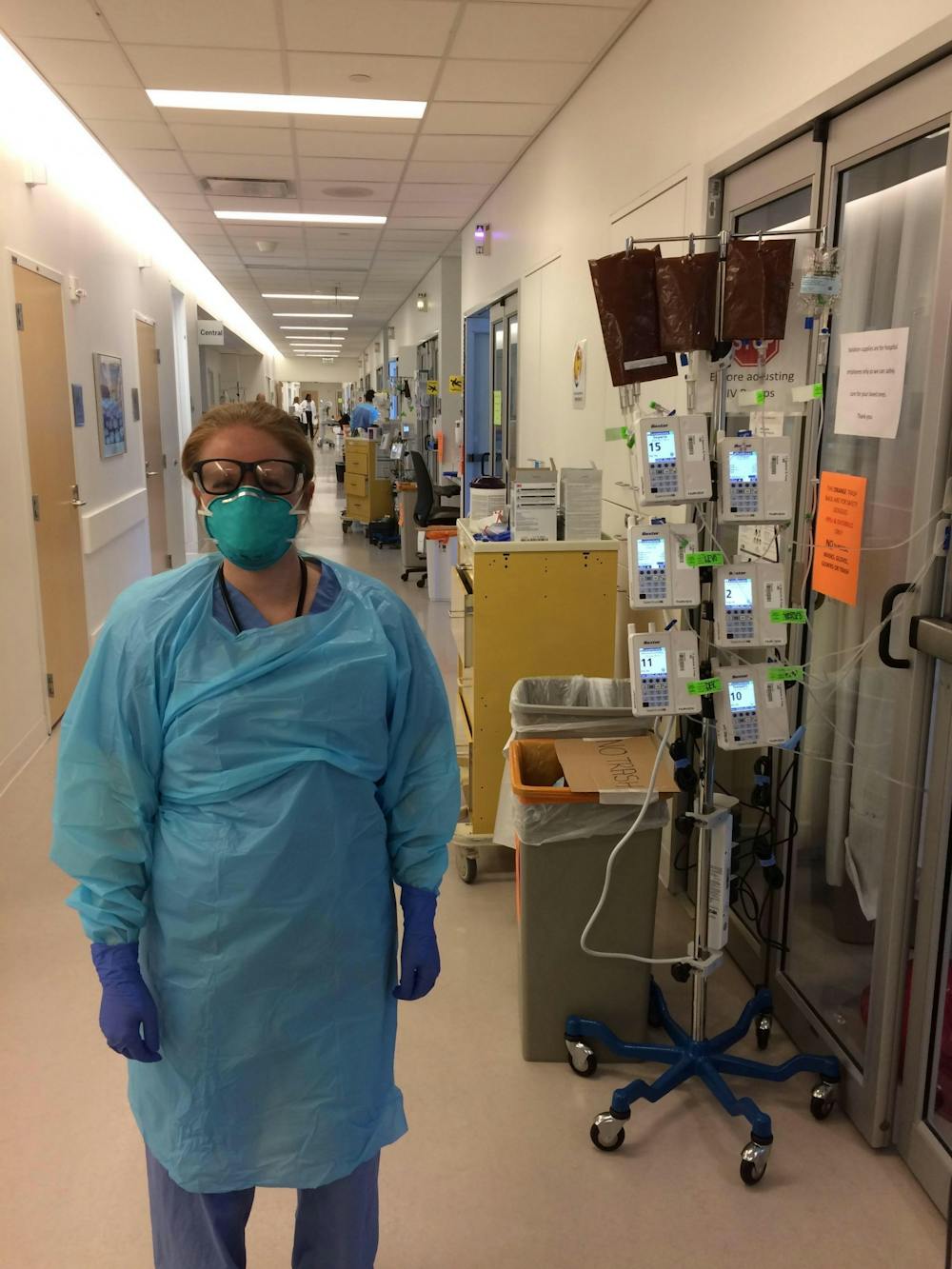
CLEVELAND, Ohio – The world is fighting an invisible battle in which those on the frontlines wear a new armor — scrubs and stethoscopes.
Life as a nurse has been both challenging and rewarding for Taylor University graduate, Katie James (’07), who has clocked in her hours for the past nine years at Fairview Hospital in Cleveland, Ohio.
As the spread of COVID-19 has brought unprecedented changes to James’s life as a nurse, her adaptability, first cultivated during her years growing up, has taken on new dimensions.
James grew up in La Paz, Bolivia where her desire to work as a healthcare professional first took root.
“Ever since I was five, I somehow always had a desire to be in medicine,” James said. “I always thought I wanted to be a doctor. I think when I was about 10 was when we started doing a lot of Matthew 28 trips.”
In partnership with local churches, teams of volunteers and healthcare professionals, the Matthew 28 trips sought to care for both the physical and spiritual needs of rural communities.
“We were trying to be the hands and feet of Jesus into rural communities,” James said. “We would go to different remote villages within Bolivia, usually within a few hours of the city (of La Paz), and we (would) go to places that hadn't seen doctors or dentists in years to bring medical help to people, but then also to have an opportunity to share the Gospel.”
At the age of 12, James was given the opportunity to shadow doctors as they saw patients, gave diagnostics and prescribed medications. She recalled the adrenaline rush she felt.
From her diverse life experiences, James developed the capacity to adapt to changing situations with grace and grit.
One of these big life changes was moving from the city of La Paz to the cornfields of Upland. James graduated from Taylor in 2007 with a degree in Bible.
Upon graduation, she went to nursing school in Cleveland, Ohio on an accelerated track while also working at a nursing home.
During this season, James learned that oftentimes, grief accompanies joy in the care of long-term patients. One patient in particular will always remain close to her heart.
As James cared for an elderly woman with advanced dementia, the patient quickly became attached to James. She would roll around the facility in a Merry Walker chair, accompanying James from room to room.
While she sometimes gave other caregivers trouble, this resident was always on her best behavior for James.
“She actually passed away several years ago,” James said. “I was very attached to her. I just remember it being super hard, and I would go a lot of times after work and just sit by her bedside and stay there pretty late just so she wouldn't be alone.”
For James, seeing patients at the end of their lives was almost easier because she never knew what they were like before.
Yet, caring for long-term patients whose vibrant personalities began to fade away was a much harder situation to watch.
“There (are) certain situations in healthcare (where) I've seen people pass away in hospitals, but sometimes you don't get as attached,” James said. “Some of those patients were only seen at the very end of their lives. But (for) some of the other people you have already grown attached to, it's a lot harder to see that grieving process.”
In August 2010, James graduated from nursing school, taking the many lessons she learned to the Fairview Hospital in March 2011.
For nine years, James has worked on the same medical-surgical floor with many of the same co-workers.
Yet, in recent months, predictability and routine have been among the many things caught in the relentless whirlwind of COVID-19. New challenges seem to arise every day.
“My co-worker initially tested negative and then just recently tested positive,” James said.
On the three to four days James is off from work, she is checking in with her co-workers for changes in policies and procedures she missed. She is met with a flood of information and emails.
The one-minute huddles that used to begin the day are now 10 minutes. Day and night shift nurses, along with management, meet to talk about high risk patients, potential issues or new updates. At times, there are multiple huddles throughout the course of the day.
“Every day is so different,” James said. “It is hard to really predict what one day is going to look like to be honest with you. (At first), every single day and sometimes multiple times a day, (management) would change policies. They would change procedures. They would change what we were doing.”
All the current and potential COVID patients are kept together to keep other patients from getting infected.
James and her co-workers wear plastic gowns, gloves, masks and goggles until they know whether the patient tests positive or negative.
“That's how we have to go into the rooms until we know if they test positive or negative,” James said. “It almost feels like you scratch one of those mystery boxes and that scratch reveals the whole day. You don't know if these patients have COVID or not, and then kind of as the day progresses, it comes back if they tested positive or negative.”
Unfortunately, the mystery box has been wrong. Patients who originally tested negative have later returned positive. Instead of immediately moving the patients to another floor, the hospital staff now keeps them on the same floor, especially if symptoms continue.
The rooms are private, which means potential COVID patients are safe from interactions with infected patients.
To stay safe, the gowns and gloves are thrown away while the goggles and masks are recycled. The Cleveland Clinic sends all of the protective equipment to be sterilized.
“They're actually sending all this stuff now to a plant where they're going to sterilize everything, so everything that's from the clavicle up gets thrown into these orange bags,” James said. “They take them somewhere to sterilize everything so that we can eventually reuse them if we need to.”
Due to the steady increase in COVID-19 patients in the intensive-care unit (ICU), many hospitals are adapting their training to quickly equip nurses to become ICU nurses.
James participated in one such training. A preparation course that normally takes three months was reduced into a six-hour class followed by a 12-hour shift shadowing an ICU nurse.
James has offered to volunteer to help understaffed hospitals in Michigan, Chicago and New York, because she is willing to take her skills where there is the most need. When she is not in the hospital, James continues to prepare herself by attending classes and researching the latest COVID-19 findings.
As James and all the other healthcare professionals continue to fight the invisible battle against COVID-19, prayers of protection and perseverance go out for each warrior on the frontlines.

Nurses on duty during the COVID pandemic.